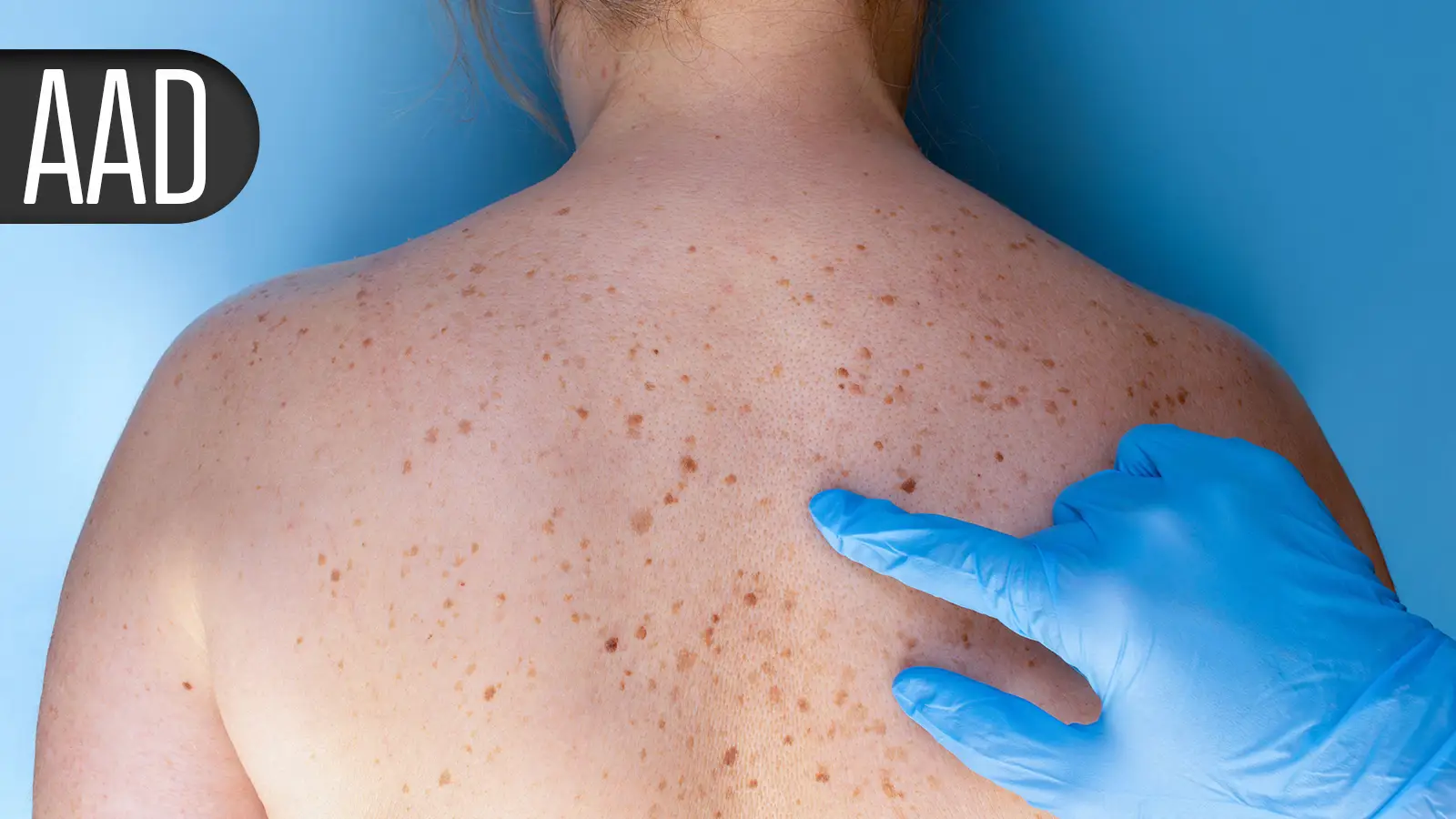
DENVER — Two drug candidates to expand oral therapy options for psoriasis had similar and consistent performances in separate phase III clinical trials reported here.
The allosteric TYK2 inhibitor zasocitinib achieved at least 75% improvement in the psoriasis area and severity index (PASI 75) and physician-rated clear or almost clear skin (physician global assessment [PGA] 0/1) in 70-75% of patients at 16 weeks in two randomized trials. In contrast, patients randomized to apremilast (Otezla) had PASI 75 and PGA 0/1 rates of below 40% at 16 weeks.
Envudeucitinib, another allosteric TYK2 inhibitor, also achieved PASI 75 in 70-75% of patients at 16 weeks and PGA 0/1 status in about 60%, as compared with PASI 75 in about 40% of patients in an apremilast control group and PGA 0/1 in 25%.
Evidence of response emerged within 4 weeks with both agents, which were generally well tolerated and produced no new safety signals as compared with earlier studies, according to reports at the American Academy of Dermatology meeting.
“[Zasocitinib offers a] once-daily, highly selective, potent TYK2 inhibitor that showed rapid responses, reproducible responses, and durable skin responses,” said Melinda Gooderham, MD, of Queen’s University in Kingston, Ontario, adding that the safety and lab profile are consistent with what is known about the TYK2 mechanism.
“We had clear skin [PGA 0] in one-third of patients treated with zasocitinib by week 16. For those patients who stayed in therapy, we saw a maintenance of response in more than 90% of patients past week 40. The patients also had superior quality of life [as compared with placebo],” she added.
Although PASI 75 was a primary endpoint of the ONWARD1 and ONWARD2 trials of envudeucitinib, the PASI 100 and PGA 0 rates (about 30% at 16 weeks) impressed principal investigator Andrew Blauvelt, MD, of Blauvelt Consulting in Annapolis, Maryland. Both outcomes continued to increase from week 16 to week 24 without evidence of a response plateau.
Zasocitinib Trials
Zasocitinib is 1 million-fold more selective for TYK2 versus JAK1, JAK2, and JAK3, which allows the drug to maintain 24-hour continuous inhibition of interleukin (IL)-23 and other immune pathways that drive psoriasis pathology, said Gooderham. The agent had demonstrated tolerability and efficacy in a phase IIb trial of patients with moderate/severe plaque psoriasis, leading to the phase III LATITUDE-PsO-3001 and 3002 randomized, apremilast- and placebo-controlled trials.
In the 3001 trial, 697 patients were randomized 3:1:1 to zasocitinib, apremilast, or placebo, and investigators in the 3002 trial randomized 1,108 patients 2:1:1 to the same three treatments. The co-primary endpoints in both trials were static PGA 0/1 and PASI 75 rates at 16 weeks for zasocitinib versus the placebo arm.
In the 3001 trial, the 16-week PGA 0/1 rates were 71% for zasocitinib, 11% for placebo (P<0.001), and 32% for apremilast (P<0.001). PASI 75 rates at 16 weeks were 76% for zasocitinib, 12% for placebo (P<0.001), and 37% for apremilast (P<0.001). In 3002, the proportion of patients achieving PGA 0/1 at 16 weeks was 69%, 13% (P<0.001), and 30% (P<0.001), and the PASI 75 rates were 71%, 12% (P<0.001), and 33% (P<0.001).
Envudeucitinib Trials
Acknowledging deucravacitinib (Sotyktu) as the first TYK2 inhibitor approved for psoriasis, Blauvelt said next-generation envudeucitinib’s greater specificity for TYK2 avoids many of the side effects associated with classic JAK inhibition. The drug’s primary effect is on IL-23 but it also blocks IL-12 and type 1 interferon signaling. Like zasocitinib, envudeucitinib affects 24-hour target blockade.
Recently, the phase II clinical trial STRIDE and its open-label extension demonstrated a favorable benefit/risk profile for envudeucitinib and meaningful clinical efficacy through 52 weeks.
Now, in the larger and identically designed ONWARD1 and 2 trials, investigators had a total of 1,771 patients with moderate/severe plaque psoriasis, randomized 2:1:1 to twice-daily envudeucitinib, placebo, or apremilast. The co-primary endpoints were PASI 75 and static PGA 0/1 at 16 weeks for the comparison of study drug versus placebo.
The primary analysis for ONWARD1 showed 16-week PASI 75 rates of 76.5% for envudeucitinib, 18.7% for placebo (P<0.0001), and 44.4% for apremilast (P<0.0001). Corresponding 16-week PGA 0/1 rates were 61%, 10% (P<0.0001), and 26.5% (P<0.0001). In ONWARD2, envudeucitinib led to PASI 75 skin clearance in 70.4% of patients at week 16 as compared with 11.7% for the placebo group (P<0.0001) and 38.6% for apremilast (P<0.0001). PGA 0/1 rates at 16 weeks were 57.3%, 5.7% (P<0.0001), and 27.4% (P<0.0001).
Improvement in scalp psoriasis with envudeucitinib mirrored the overall improvement in terms of rapidity and extent of improvement, said Blauvelt. Itch scores began to improve as early as 2 weeks after starting treatment.
In response to a question from the audience, Blauvelt acknowledged a theoretical possibility for tuberculosis reactivation with the TYK2 inhibitor’s effects on both IL-23 and IL-12. Whether the risk is real remains to be seen. In response to another question, he said investigators saw nothing unusual in terms of the frequency or type of infections that occurred with envudeucitinib.
Source: Read Full Article