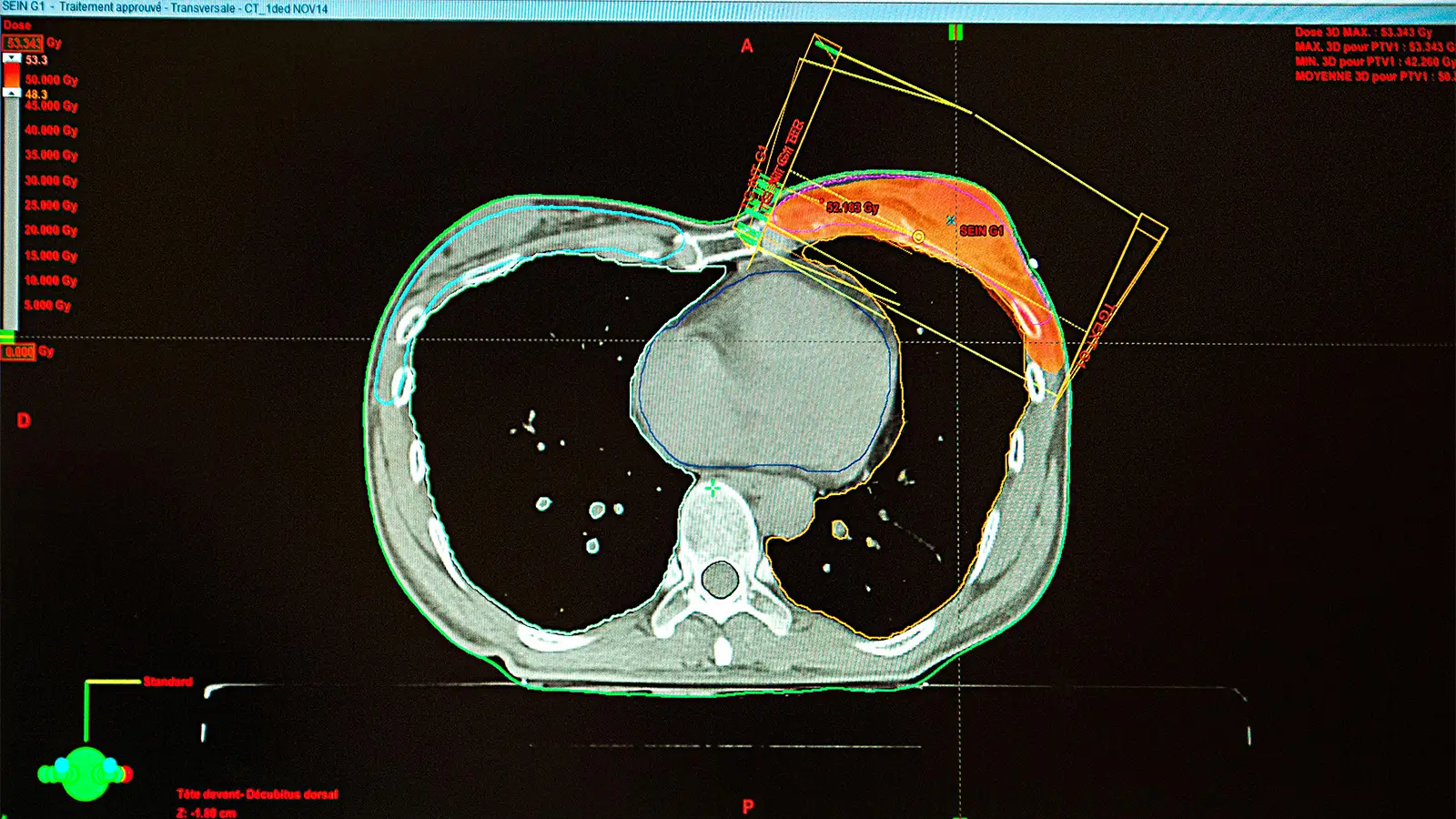
- Women with left-sided breast tumors historically have had an increased risk of cardiovascular disease due to use of radiation therapy.
- In a retrospective study, there was no difference in the 15-year cumulative incidence of first heart disease hospitalization between women with left- and right-sided breast cancer.
- Among women with pre-existing heart disease, new diagnoses of heart failure and ischemic heart disease were slightly more common after left-sided radiation.
Contemporary external beam radiation therapy (EBRT) techniques appear to have reduced the risk of cardiovascular disease (CVD) among women with left-sided breast cancer, a large retrospective cohort study suggested.
Among women treated with photon-based EBRT from 2002 to 2017, the 15-year cumulative incidence of first CVD hospitalization was 13.8% in those with left-sided breast cancer versus 13.5% in those with right-sided breast cancer (P=0.43), reported Husam Abdel-Qadir, MD, PhD, of Women’s College Hospital in Toronto, and colleagues.
After adjusting for baseline covariates, tumor laterality was not significantly associated with the hazard of hospitalization for CVD (HR 1.02, 95% CI 0.98-1.06, P=0.36), they wrote in JAMA Network Open.
Breast radiotherapy techniques used before the 1980s exposed surrounding organs to large doses of radiation, so women with left-sided tumors historically received higher mean heart doses than women with right-sided tumors, which increased their risk of coronary artery disease, cardiomyopathy, valvulopathy, arrhythmias, and pericardial disease.
The findings in this study “provide population-level reassurance that modern radiation techniques have largely mitigated the excess long-term cardiovascular mortality and morbidity historically associated with left-sided [breast cancer] treatment for women with typical radiation exposure,” Abdel-Qadir and colleagues noted.
However, for women with pre-existing CVD, new diagnoses of heart failure were slightly more common after left-sided EBRT (10.2% vs 9.6%, P=0.01), as were new diagnoses of ischemic heart disease (13.6% vs 12.8%, P=0.03). The rate of CVD hospitalizations when including recurrent events was slightly higher for left-sided disease (1.72 vs 1.63 per 100 person-years, P=0.006).
In a commentary accompanying the study, Avirup Guha, MD, MPH, of the Medical College of Georgia at Augusta University, noted that when it comes to counseling patients regarding breast radiation therapy and cardiovascular risk, clinicians should emphasize patient-specific absolute risks.
“For patients with low baseline CVD risk and low anticipated cardiac exposure, the incremental absolute risk from contemporary radiotherapy may be very small, often outweighed by oncologic benefit,” Guha wrote. “For patients with high baseline risk or higher expected cardiac exposure, the same relative effect can translate into a larger absolute excess risk, making cardiac-sparing imperative.”
For this population-based study, Abdel-Qadir and colleagues used administrative health databases in Ontario, Canada, to identify women who received EBRT after a diagnosis of unilateral breast cancer from April 2002 through December 2017. They were followed up through February 2025 for most outcomes, and through December 2022 for cause-specific mortality.
The 76,586 women included in the study had a mean age of 59, and 50.2% had left-sided tumors.
During a median follow-up of 10.9 years, there were a total of 14,370 hospitalizations for CVD, 8,432 hospitalizations for heart failure, 2,575 hospitalizations for acute myocardial infarction, 2,444 hospitalizations for stroke, and 652 hospitalizations for pericardial disease.
Among 71,675 women without CVD before their first radiation treatment, there were 8,368 new diagnoses of ischemic heart disease, 6,013 diagnoses of atrial fibrillation, and 6,204 diagnoses of heart failure.
Twenty-three percent of patients died, with no difference in all-cause mortality at 15 years between women who underwent left- or right-sided EBRT. There was no difference in major adverse cardiovascular events between the groups, including acute myocardial infarction and stroke.
Radiation-associated CVD risk may be more relevant for older women and those who received chemotherapy, the authors noted.
Among women younger than 50 years, left-sided tumor laterality was significantly associated with increased risk of CVD at 15 years (4.8% vs 3.9% for right-sided laterality, P=0.02), but there was no significant difference among women 50 and older.
For women who received chemotherapy, left-sided tumor laterality was significantly associated with an increased risk of CVD at 15 years (11.3% vs 10.3%, respectively; P=0.01), with no significant difference among women who did not receive chemotherapy.
Abdel-Qadir and colleagues acknowledged that the study had several limitations. For example, since they used administrative data, they did not have access to treatment characteristics, including radiation doses to the heart, or treatment plans, and they were also unable to differentiate between patients who received partial breast versus whole breast radiation therapy. They also did not assess subclinical or imaging-based cardiac injury.
Source: Read Full Article